Cancer radiation therapy is a double-edged sword. Cancer cells must be accurately destroyed using high-energy radiation, but surrounding normal tissue must be saved as much as possible. In this case, ‘assistive devices’ play a surprisingly big role. Increasing the precision of cancer treatment and reducing side effects.
Professor Jihoon Choi’s team in the Department of Radiation Oncology at Samsung Changwon Hospital recently applied for patents for three patient-centered assistive devices. It is a bolus that adheres better, a bolus that shows the condition in color, and a fixture that notifies changes in the oral environment in advance.
Bolus is a special transparent pad that is placed on the skin. It looks like a soft silicone gel pad. When treating tumors close to the skin, such as breast cancer or skin cancer, it helps the radiation sufficiently reach the surface and adjusts it to fall exactly at the desired depth. It is a thickness-customized cushion that fine-tunes the ‘focus’ and ‘depth’ of radiation.
It is still widely used in clinical settings. However, because the degree of skin adhesion was different depending on the patient’s body type and lesion location, there were limitations that made it difficult for medical staff to immediately check.
“The bolus adheres closely, indicates color, and sounds an alarm in advance.”
The ‘vacuum compressed bolus’ developed by Professor Choi’s team has a structure that adheres tightly to the skin. This is because when the air is removed with a vacuum, the bolus changes shape to match the patient’s body shape. Therefore, stable treatment is possible even in a lying position (prone position) without having to lie down.
Superficial tumors on the back or lower back are usually treated lying prone. However, there are patients who have difficulty lying down due to their body type or medical problems, and this problem can be solved.
It can be restored to its original form by releasing the vacuum after use. Then, it can be reused for the same patient, reducing the disadvantages of boluses such as high cost and disposable use.
‘Thermochromic discoloration bolus’ is also special. It uses a material that changes color by detecting temperature changes and becomes transparent when properly adhered to the skin. If the color disappears, it is well attached. Medical staff can check at a glance.
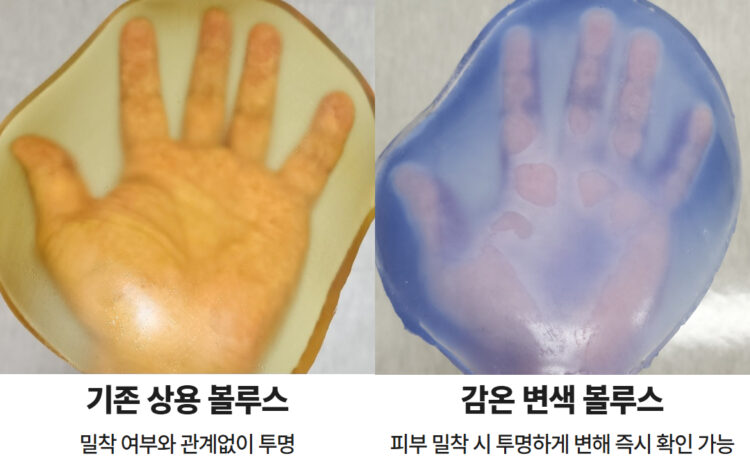

On the other hand, the color remains in the areas where air remains due to lack of adhesion. If such poor adhesion occurs, radiation leakage occurs and treatment effectiveness decreases due to insufficient dose.
Additionally, if the skin temperature rises rapidly during treatment, it turns red. This allows for early detection of unexpected skin irritation or possible damage.
The key point of the third item, ‘smart oral fixture’, is that it shows changes in ‘acidity (pH)’ in the mouth through color. Radiation treatment for head and neck cancer or oral cancer can cause inflammation or damage to the mucous membrane of normal tissues in the oral cavity.
In such cases, a function that changes color according to changes in pH in the mouth was installed in the device to detect the risk of mucosal damage early. Preemptive response to side effects is possible. It can also reduce the risk of treatment interruption or delay.
Why ‘assistive devices’ determine the success or failure of treatment
Radiation is dangerous, so a difference of 1 mm can determine the effectiveness of treatment and its side effects. If the bolus is not well adhered to the affected area, the distribution of radiation dose is disrupted, and if the skin overheats, the risk of burns or inflammation increases. Additionally, if the oral mucosa is damaged, the patient’s nutritional status deteriorates rapidly due to pain and the inability to eat. Treatment is inevitably delayed.
In that respect, these three types of patents are designed to make these on-site risks ‘visible’ and ‘relax posture constraints’ to prevent problems in advance. There are various side effects, such as increasing patient convenience and reducing treatment costs.
It can be said to be a patient-centered idea that “improves the quality of radiation therapy in places that were previously invisible.” Accordingly, Professor Choi Ji-hoon’s team said on the 4th, “We will continue patient-centered research and development to ensure that patients receive precision treatment more comfortably.”



